Useful
Living with Scleroderma
Living with scleroderma can be a challenge at first but we have put together some tips and ideas that will help you get started.
Scleroderma is a chronic skin disease, meaning it does not go away, yet it can be treated. The term scleroderma comes from the Greek words skleros (hard) and derma (skin) and is a disease characterised by progressive skin hardening that can make the skin look like leather. The tightening of the skin can also reduce the range of movement of joints. Scleroderma is a connective tissue disease that also involves subcutaneous tissue, muscles, and internal organs including the gastrointestinal tract as well as the respiratory, renal, cardiovascular, musculoskeletal, endocrine, and genitourinary systems.
The most commonly affected parts of the skin are the areas around the elbows and knees but can also affect the face and neck. Diffuse scleroderma is when the skin thickens on the torso, hands, and feet as well as the face.
Research is continuing into the causes of scleroderma, which are considered to be complex. Increasing evidence suggests that a combination of environmental and genetic factors play a part, with some changes being found in a patient’s DNA expression to cause an autoimmune reaction. However, it is not yet clear how these are all related during the development and progression of the disease.
Whilst scleroderma is not an inherited disease, a genetic predisposition plays an important role in its development. Environmental factors can trigger or accelerate the disease in those who are susceptible. These factors include exposure to silica or solvents as well as exposure to radiation or radiotherapy.
The incidence of scleroderma varies between countries. In the United States, the rate is 20 cases per million population, though there appears to have been an increase over the past few decades even when factoring in better diagnosis rates. The disease also appears to have different rates within ethnic groups, with black people affected more than white people. The risk is also much higher for men than women, though it is still unclear why this is so. Whilst children and older people can be affected, it usually appears in individuals between the ages of 30 and 50 years.
Signs and symptoms of scleroderma may involve the following systems:
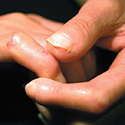
In scleroderma, the skin can at first become puffy (oedema), which do not respond to diuretic therapy, before becoming tight and hard. First, the fingers are affected before spreading into the hand.
The skin on the face can become tighter, which removes any wrinkles and there may be skin pigment changes, with skin becoming either lighter or darker.
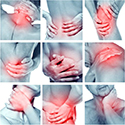
Joint pain can be either arthralgia or myalgia. The terms arthralgia and myalgia are often used in combination or interchangeably. Arthralgia is defined as pain in a joint whereas myalgia is generalised muscle pain. There may be a reduction in the range of movement or flexion. Other signs are symptoms of carpal tunnel syndrome or muscle weakness.
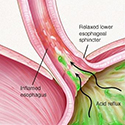
Gastroesophageal reflux, otherwise known as heartburn or acid indigestion is one sign as well as indigestion (dyspepsia), bloating or feeling full after only a small amount of food. There may be constipation alternating with diarrhea leading to malnutrition.
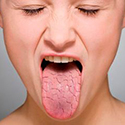
This manifests as Sicca syndrome, also called Sjogren's syndrome, which classically combines dry eyes, dry mouth, and another disease of connective tissue such as rheumatoid arthritis. Teeth can also become loose.
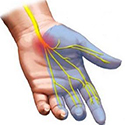
Facial pain and decreased sensation. Pins and needles sensation (paresthesias) and weakness in the hand. Headaches, depression, and anxiety. It can also lead to tiredness, weight loss and loss of appetite.
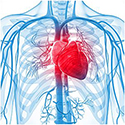
Shortness of breath due to heart problems. Palpitations, irregular heartbeat, and fainting (syncope) due to abnormalities in the heart, for example, when the heart beats to slow or too fast (arrhythmia).
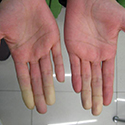
Reduced blood flow in the fingers is often seen as the first sign of scleroderma. There may be ulcers on the fingertips. Visibly dilated blood vessels (telangiectasias) are also a sign.

Erectile dysfunction, Vaginal narrowing, dryness, and pain caused by vaginal fibrosis (too much connective tissue) or bladder fibrosis. Difficult or painful sexual intercourse (dyspareunia).

Progressive shortness of breath (dyspnea) and pain in the chest wall (precordial chest pain) and a persistent dry cough.
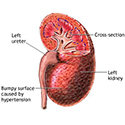
Hypertension or the kidneys not working well.
Whilst a doctor can make a diagnosis of the physical symptoms, they will also ask for tests to follow up. These will include blood tests to check enzyme and autoantibody levels and tests to assess the involvement of any internal organs.
For gastrointestinal checks, this would require a simple X-ray, biopsy or colonoscopy. For involvement of the heart and lungs an ECG and computed tomography scan is usually offered, and if the disease is active in the area, these are repeated every six months
Symptoms can be managed with the use of non-steroidal anti-inflammatory drugs like ibuprofen or aspirin to help with swelling and pain. Steroids help control the immune response to help with muscle, joint, or internal organ problems. There are also drugs that boost blood flow to your fingers, blood pressure and heartburn medications as well as lotions and potions to help prevent tissue from scarring.
The children of Margaret Rowland Plowden, Louise Burns and Earle Rowland made a generous gift to the MUSC Division of Rheumatology in 2011 to advance scleroderma research. Аfter the death of their mother who fought a long and inspiring battle against a terrible disease, scleroderma.
What to get your boyfriend for Valentine's day is always a hard question, especially when we talk for people with Scleroderma. We have some suggestions like special slippers or shower shoes, pill day organizer, heated socks or heating pads are good ideas.
The UK is fortunate in being home to some of the world’s leading experts on scleroderma, most of whom are housed in departments of rheumatology in leading teaching hospitals […]
Specialist scleroderma clinics are vital to ensure the best care and treatment of scleroderma patients, as well as patients with rare diseases sharing some of the signs and symptoms […]
Copyright © All Rights Reserved - sclerodermasociety.co.uk